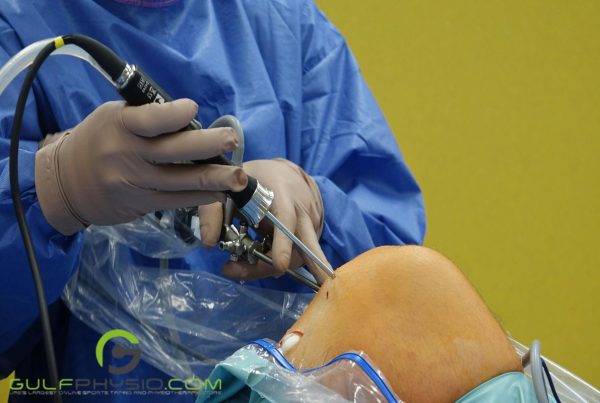
Knee osteoarthritis is a condition that causes the cartilage in the knee to become worn and damaged. This can make walking, climbing stairs, or even standing difficult. If you’re experiencing pain in your knee, you might want to consider discussing knee osteoarthritis with your doctor.
This article discusses the causes of knee OA, the different types of OA, and the best ways to treat and manage the condition.
What Is Knee Osteoarthritis?
In terms of knee arthritis, osteoarthritis is the most common type. Knee osteoarthritis is degenerative, “wear and tear” form of arthritis that typically affects persons over 50. However, it can affect people of any age.
The progressive degeneration of knee cartilage characterizes knee osteoarthritis. Cartilage wears down over time, leaving less cushioning space between bones. When bones rub against one another in this way, painful bone spurs can form.
As time goes on, the discomfort from knee osteoarthritis only increases in severity.
Anatomy
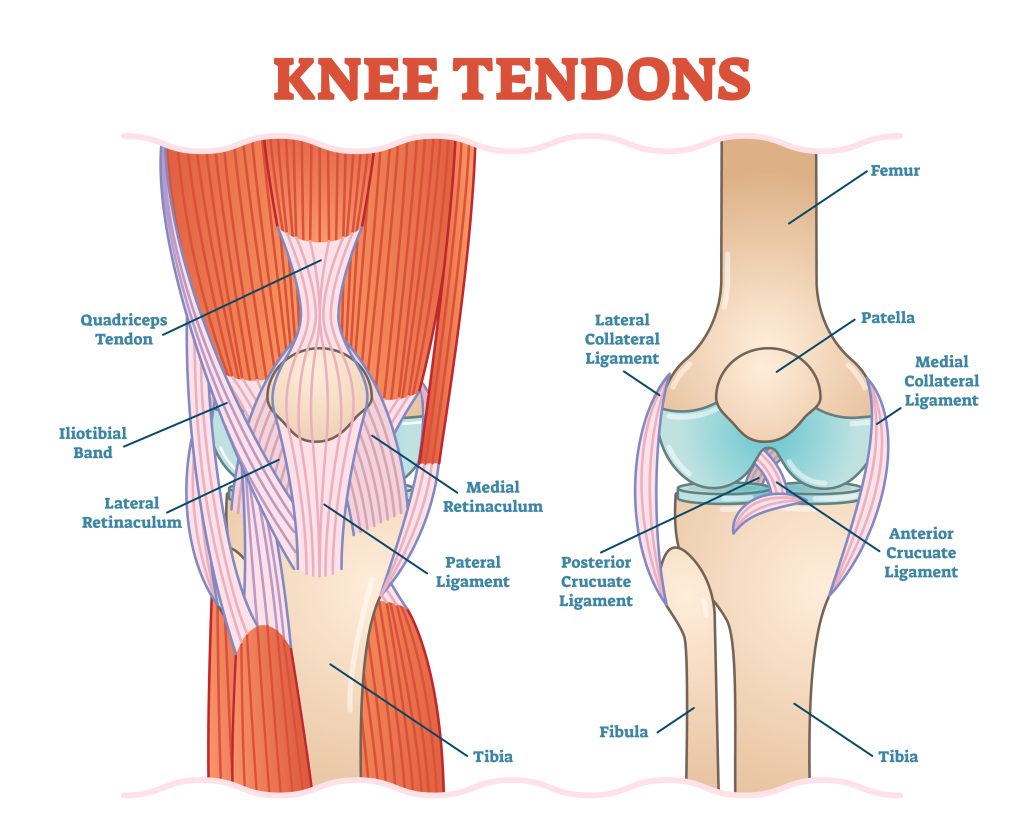
The knee is the biggest and most powerful among the body’s joints. The patella, tibial plateau, and distal femur all contribute to the structure of the knee (kneecap). Articular cartilage is a smooth, slippery substance that covers the ends of the three bones that make up the knee joint. It cushions and protects the knee bones as they bend and straighten. In between the thighbone and shinbone are two wedge-shaped cartilage pieces called menisci. They are robust and springy to provide shock absorption and joint stability. The synovial membrane is a very thin lining that covers the inside of the knee joint. This membrane secretes a fluid to keep the cartilage from wearing out too quickly.
What Are Risk Factors Of Osteoarthritis Of The Knee?
- Age. As we age, our cartilage and synovial fluid, which keep our joints lubricated, naturally break down and age. This makes us more likely to get osteoarthritis.
- Past injury. A history of joint injuries, especially to the knee, can raise the likelihood of getting OA later in life.
- Genetics. Cartilage formation can be more challenging for certain people.
- Obesity. Extra weight places great strain on your knees and other weight-bearing joints.
- Occupation. The most common occupations that cause knee pain are construction, childcare, gardening, mining, and flooring specialists.
- Sports. High-impact athletes like pitchers, linemen, ballet dancers, and runners are also at risk.
Symptoms of Knee Osteoarthritis
- Knee pain, especially first thing in the morning, goes away within half an hour at the most
- Knee stiffness from sitting or sleeping for long periods
- Pain that worsens with movement and improves after sitting still
- The discomfort felt upon applying pressure on the knee
- Signs of knee joint distress, such as cracking, creaking, or crunching
- A feeling of the knee locking or catching sensation
- The sensation of a growing bone spur near the joint
- Difficulty performing routine tasks, such as walking, crouching, ascending stairs, or getting in and out of a car
What Are The Five Stages Of Knee Osteoarthritis?
There are five stages of knee OA:
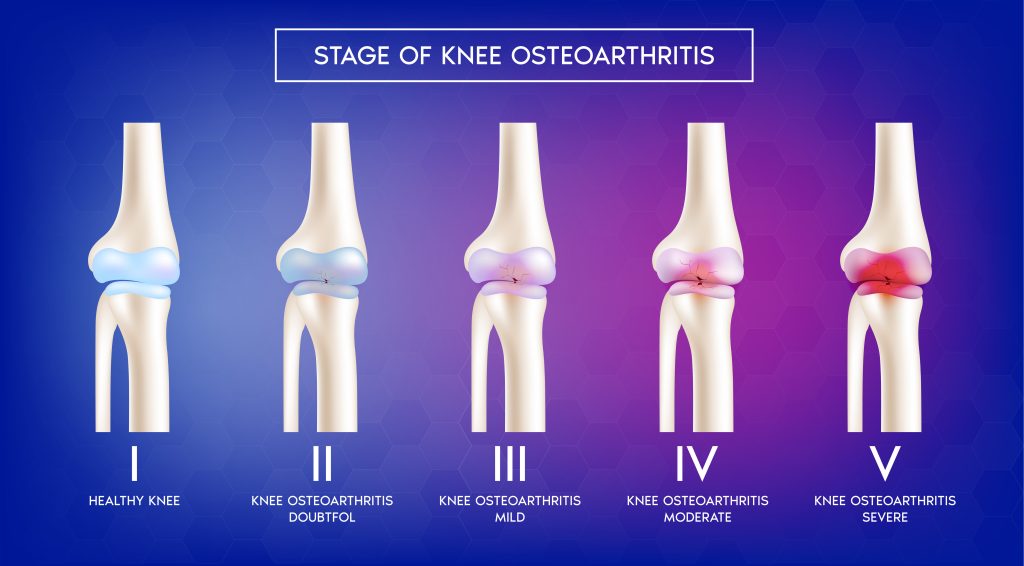
- Grade 0: In terms of knee health, this is considered “normal.”
- Grade 1: There is only a tiny bone spur, yet the patient reports no pain.
- Grade 2: This is the point at which patients first notice symptoms. After a long day of walking, they will feel increased stiffness in the joint and experience pain. Even at this early stage, X-rays will show increased bone spur growth. Therefore the issue is worse than it seems. The cartilage should keep its normal size.
- Grade 3: Moderate OA. Stiffness and discomfort in the joints will be more common after sitting for a long time. Damage to the cartilage and a narrowing of the intervertebral disc are both readily apparent.
- Grade 4: This is the worst possible OA stage. As a result, there will be much less room for movement in the joint as the cartilage and synovial fluid dry up. Extreme discomfort and pain are common during this stage, especially while walking or using the affected joint in any way.
What Is The Best Way To Diagnose Knee Osteoarthritis?
- X-rays: Joint space narrowing is a telltale sign of cartilage degeneration. An X-ray finding of osteoarthritis is not always indicative of the condition being the cause of the patient’s symptoms. Even though a joint may feel well, X-rays may show osteoarthritis. Many alternatives exist for treating osteoarthritis once it has reached a more advanced stage.
- Magnetic resonance imaging (MRI): An MRI scan shows cartilage and other soft tissues in detail. It’s not common to use an MRI to diagnose osteoarthritis, but it can be useful in some cases.
- Blood tests: Although there’s no reliable blood test for osteoarthritis, some indicators in the blood can help rule it out.
What Is The Best Treatment For Osteoarthritis In Knees?
Although there is currently no cure for osteoarthritis, therapy can ease symptoms and improve mobility.
Medication
Several different medications can help ease knee osteoarthritis pain. Everyone reacts to medications differently, so you’ll work with your doctor to find the right combination of drugs and doses.
The first line of defense against knee arthritis is pain relievers and anti-inflammatory drugs without prescriptions. Acetaminophen, a common OTC pain medication, may help alleviate arthritic discomfort.
Therapy
Physical therapy can relieve knee osteoarthritis symptoms and slow it down. An individualized exercise and manual treatment program designed by a physical therapist helps patients with knee osteoarthritis. With this program, they can move around more freely and with less pain.
Surgical Procedures
Your doctor may suggest surgery if the pain from your arthritis makes you unable to work and other treatments don’t help. There are a variety of knee procedures, each with its own set of advantages and disadvantages. Before surgery, your doctor will talk to you about the potential risks.
Alternative Procedures For Knee Osteoarthritis
- Acupuncture is the insertion of very thin needles into certain points of the body. Pain relief and deep relaxation are the goals of this procedure.
- Stem cell injections and platelet-rich plasma (PRP) are methods for treating joint pain that involve reinjecting cells from the patient.
- The PRP treatment involves extracting platelets from blood and concentrating them, then injecting them into the knee. There’s been a link between platelet growth factors and reduced inflammation.
- It’s possible to get the precursor cells out of a patient and inject them into the knee. Since these are primitive cells, there is hope they can develop into new tissue and repair worn-out cartilage and bone.

Role Of Physiotherapy for Knee Osteoarthritis
Exercises
Stretching and strengthening exercises for the legs will help you move more freely and more easily. Physical therapists and doctors can work with you to create a tailor-made fitness plan.
- Low-impact aerobic exercise: Improving cardiorespiratory fitness and general health through low-impact activities like swimming or riding a stationary bike.
- Strengthening exercises. The exercises strengthen the hip and core and the muscles around the knee, making the joint more stable and mobile. For strengthening exercises, you can use cuff weights, resistance bands, and equipment for lifting weights.
Pain management modalities
- Use ice and heat to treat flare-ups of arthritis pain.
- Transcutaneous electrical nerve stimulation (TENS). To alleviate discomfort, this device uses a low-voltage electrical current. Some patients with osteoarthritis in the knees or hips find temporary relief.
Assistive devices
Using aids like a cane, brace, or knee sleeve may be beneficial. A brace can help with stability and function when your knee osteoarthritis is only on one side.
Taping
Like bracing, kinesio taping helps reduce joint stress, which is beneficial in the short term.
Bracing
A splint or brace may be helpful for short-term relief from severe joint discomfort. Splints can also immobilize smaller joints so they can heal. Keep your range of motion up by taking breaks from wearing a brace.
Balance and gait training
The therapist will help the patient learn strategies for staying upright and adjusting to levels changes while performing routine tasks.
Posture training
When sitting, standing, or walking, maintaining correct posture can alleviate pressure on arthritic joints.
Manual Therapy
Manual manipulations of the soft tissues and joints to improve range of motion in the knee and lessen stiffness.
Aquatic therapy
Patients with arthritis can exercise in a warm water therapy pool with less pain and more freedom of movement. The warm water makes it easier for the joints to support your weight, reduces inflammation, and gives you temporary pain relief.
Lifestyle education and changes
A change in lifestyle can help alleviate knee pain and prevent further damage. Maintain a healthy weight, move the knee often to prevent stiffness, wear shoes with adequate arch support, and don’t sit for more than 30 minutes.
What Should You Not Do With Osteoarthritis Of The Knee?
Overuse or direct trauma to the affected joint are the most typical causes of an OA flare. Potential causes include bone spurs, stress, repeated motion, cold weather, a shift in barometric pressure, an infection, and weight gain.
A Note From Gulf Physio
We hope you’ve enjoyed learning about the subject matter above. This blog post is not a substitute for medical advice. The author cannot guarantee the accuracy of the information presented. If you have any questions or concerns, please consult a healthcare professional. All decisions and actions you make are your own. No one involved in making this resource is liable for its use.