
Waking in the morning, you need to start your day on the right foot. Sadly, taking your first few steps, you can feel this stabbing pain around your heel. It might disappear after a couple of steps, but it always comes back. Knowing this, chances are you have plantar fasciitis.
Plantar fasciitis is a prevalent source of heel pain. In this article, we’ll delve into the symptoms and possible treatment options for this condition. But first, let’s find out what plantar fasciitis is.
What is Plantar Fasciitis?

Also known as runner’s heel, plantar fasciitis happens when the plantar fascia is inflamed. The plantar fascia is the long ligament connecting the front of your foot to your heel. It cushions the sole of your feet which also means that it deals with the brunt of your foot’s work.
As you can tell, plantar fasciitis happens when someone overuses that part of their feet. Although physical therapists and physiotherapists alike treat many foot conditions like plantar fasciitis, diagnosing them is a different matter.
How Do You Diagnose Plantar Fasciitis?
The patient’s medical history will be taken into consideration when diagnosing plantar fasciitis. A history of progressive pain in that area, particularly at the medial and inferior heel, will raise some flags.
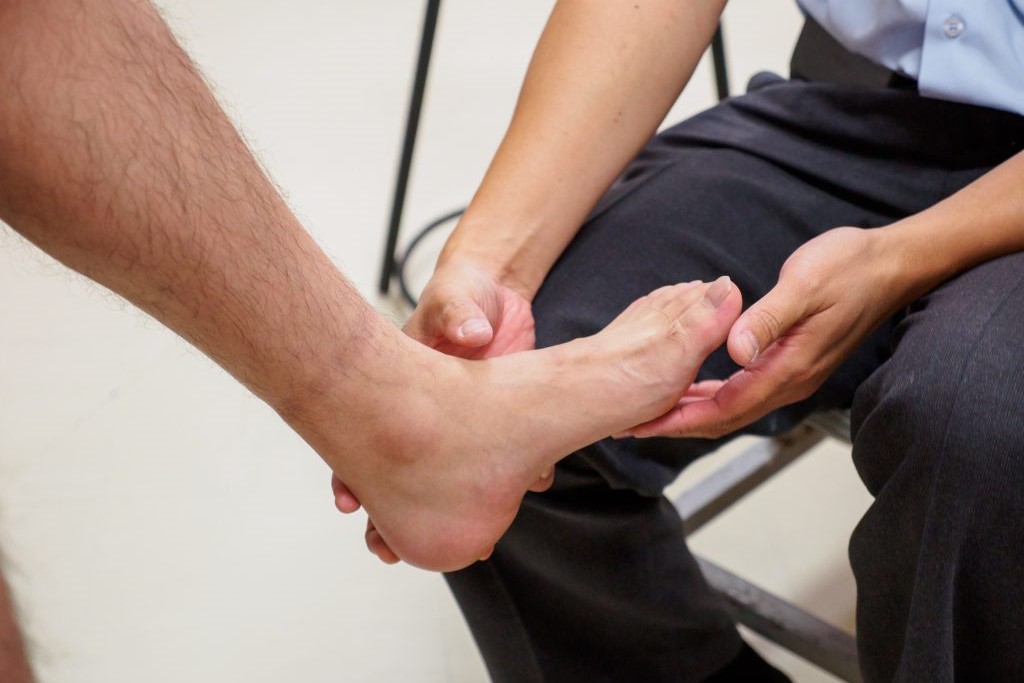
Next, a thorough physical exam from a healthcare professional will determine whether a person has this condition or not. They will check for any feelings of tenderness in your foot. Knowing the location of the said tenderness might help determine the cause of the pain. Apart from the tenderness, here are the other signs your podiatrist will look for:
- You experience discomfort while standing or walking, but it stops after a few steps
- You may feel a slight tenderness in the middle of the foot right under the heel bone
- You might notice some swelling at the bottom of your foot if you press on area
- You experience some pain when you bend your foot upward or stand on tiptoe
In terms of imaging tests, it’s usually not needed for a condition like this. However your doctor might recommend such tests to determine whether another injury could be causing the pain. Examples of said injuries are stress fractures and tendon ruptures.
What Are the Risk Factors of Plantar Fasciitis?

There are a variety of risk factors associated with plantar fasciitis. They can be divided into different subcategories which include the following:
The Mechanics of Your Feet
Different foot anatomies could potentially predict whether one is more vulnerable to plantar fasciitis. For example, you could end up experiencing constant foot pain if you have high arches or flat feet. It could also happen if you don’t walk or run properly.
All of the above factors interfere with the overall weight distribution on the feet. When you put too much unnecessary pressure on the plantar fascia, it could put a strain on it.
The Use of Improper Footwear
Since your feet handle the bulk of your movement and body weight, having the right support is vital. This means having the best and most comfortable shoes for the job. Your shoes need to fit well for you to do what you need to do, This is particularly important for athletes.
The two main factors you need to look for for the perfect fit are space and arch. Shoes that are too narrow like high heels, particularly on the toe and heel region, cramp up your feet. Because of this, women in general are more susceptible to foot-related pain and injuries.
When buying your next pair of shoes, consider the toe box and arch spaces. There should be adequate space in the toe box and an appropriate shape that best supports your arch shape.
The Kind and Intensity of Certain Activities
Some athletes like gymnasts or runners can put an extraordinary strain on their plantar fasciitis over time. They can develop something called microtears because of the constant effort being placed on the plantar fascia.
It’s also a risk for nonathletes during drastic changes in the intensity and duration of their regular activity levels. This can permanently harm the plantar fascia. Try to remember to warm up and stretch effectively before any workout. Don’t forget to take breaks whenever your feet start to hurt, to give yourself some time to recuperate.
The Occupation of the Individual
Generally speaking, people who spend the majority of their time on their feet have an increased risk of developing plantar fasciitis. It includes occupations like being a nurse, a teacher, or a factory worker. Any job that requires an individual to stay on their feet for long periods at risk.
Moreover, work-related weight-bearing can also increase the risk of plantar fasciitis especially when done improperly. Lifting an inordinate amount of weight for work is sometimes inevitable but any injury can be avoided. All you need is to learn the right way to lift.
The Age of the Individual
The plantar fascia can get weaker over time. Meaning, it’s more susceptible to tears and other related injuries. With that being said, there’s a higher risk of getting plantar fasciitis when you reach the ages of 40-60 years old.
The Weight of the Individual
We already know that your feet essentially carry your weight. So imagine adding an extra load to that task. Obese people might put more unwanted strain on their feet which leads them to use their feet less and less.
To take some pressure off of your feet, an effective diet-and-exercise program is recommended.



